Thanks to a $15.1 million grant to UNM Health Sciences Center from the U.S. Centers for Medicare and Medicaid, remote rural hospitals across the state will soon have the next best thing to their very own neurosurgeon.
The grant, which is the largest UNMH’s Neurosurgery Department has ever received, will go toward setting up a telemedicine network that will allow emergency room doctors in rural hospitals to connect directly with neurosurgeons at UNM Hospital. They can then assist with diagnosing traumatic brain injuries, strokes, and even brain tumors.
“For a small department like ours to get that kind of money is a pretty big deal,” said Susy Salvo-Wendt, unit administrator for the UNMH Department of Neurosurgery.
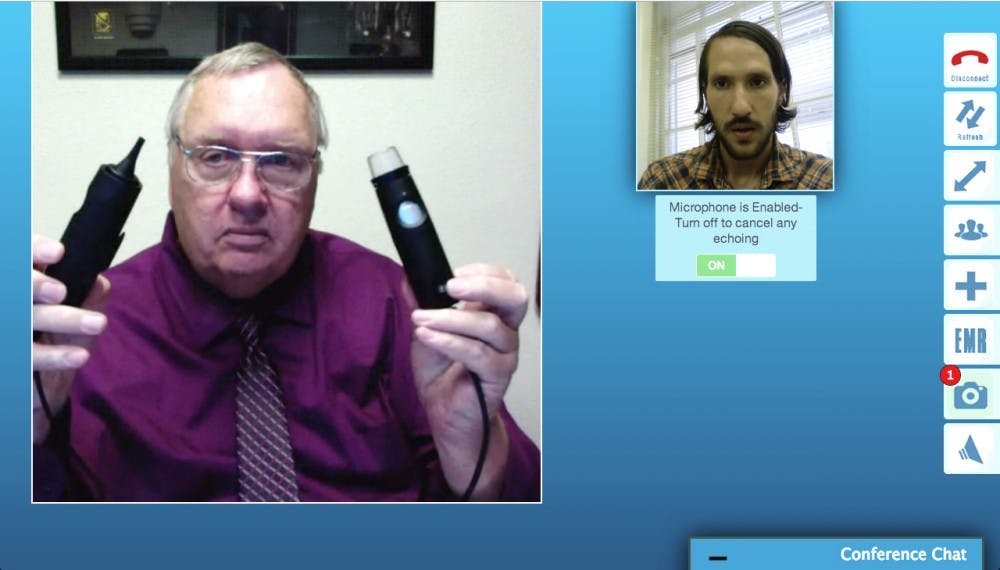
The program, called ACCESS, will provide 30 hospitals around the state with inexpensive telemedicine carts that feature a large screen and camera for conference calling, diagnostic equipment, and the ability to quickly share MRI and CT scan images.
The goal of the program is to provide small hospitals access to expertise, while at the same time saving money by avoiding unnecessary and costly emergency airlifts to UNMH.
“What we found is that a lot of people over-diagnose (patients) with traumatic brain injuries. Sometimes the doctors at these rural hospitals would get excited because they didn’t have enough experience with this, and they would fly the patients here, which is $25,000 a pop,” Salvo-Wendt said.
In the test period for this system, the team found that nearly half of the proposed airlift transfers were not needed. According to the grant proposal, the system is expected to save $20.1 million over the three years that the grant funds.
In cases where patients did need further emergency treatment, doctors were able to diagnose the problems faster and transfer the patients sooner, saving lives, Salvo-Wendt said.
The telemedicine carts being used were built by Albuquerque-based health tech company Net Medical Xpress. The units cost about $5,000 each, a fraction of what other, more complicated equipment costs, CEO Dick Govatski said.
“The interface we designed is simple and efficient,” Govatski said. “There’s no expensive software, and we don’t need a $38,000 remote controlled robot to do these kinds of things.”
Salvo-Wendt said that the rural hospitals benefit greatly from the system because the patients can stay closer to home with their families, and when they don’t need to be transferred, the insurance money for treatment will stay at these hospitals as well.
For the three years that the grant funds, the consultations will be free to these small hospitals. After that, UNMH will charge a $600 fee per consultation.
Get content from The Daily Lobo delivered to your inbox
If the program goes well, Salvo-Wendt said the greater goal will be to expand the telemedicine system, using it to diagnose many more conditions. They eventually plan to implement similar systems across the country.
“If this works, we could then do all kinds of different specialties through this system: critical care, psychiatry, dermatology, lots of other things,” Salvo-Wendt said. “Telemedicine is really the wave of the future in medicine.”
Net Medical Xpress plans to continue developing its technology as well. Govatski said that eventually the company would like to take the carts from the hospital and into the home. Patients who are unable to get to the hospital could have their own cart at home, allowing them to have regular checkups and even exams without ever leaving the house.
The grant was funded by the Department of Medicare and Medicaid’s Health Care Innovations Award, a $1 billion dollar fund created to help find innovative models that can provide better care and save money at the same time.
“We’re really trying to come up with new models for delivery of services to these rural patients,” Salvo-Wendt said. “It’s a game-changer.”
Jonathan Baca is a news editor at the Daily Lobo. He can be reached at news@dailylobo.com or on Twitter @JonGabrielB.